Cervical Disc Replacement Surgery
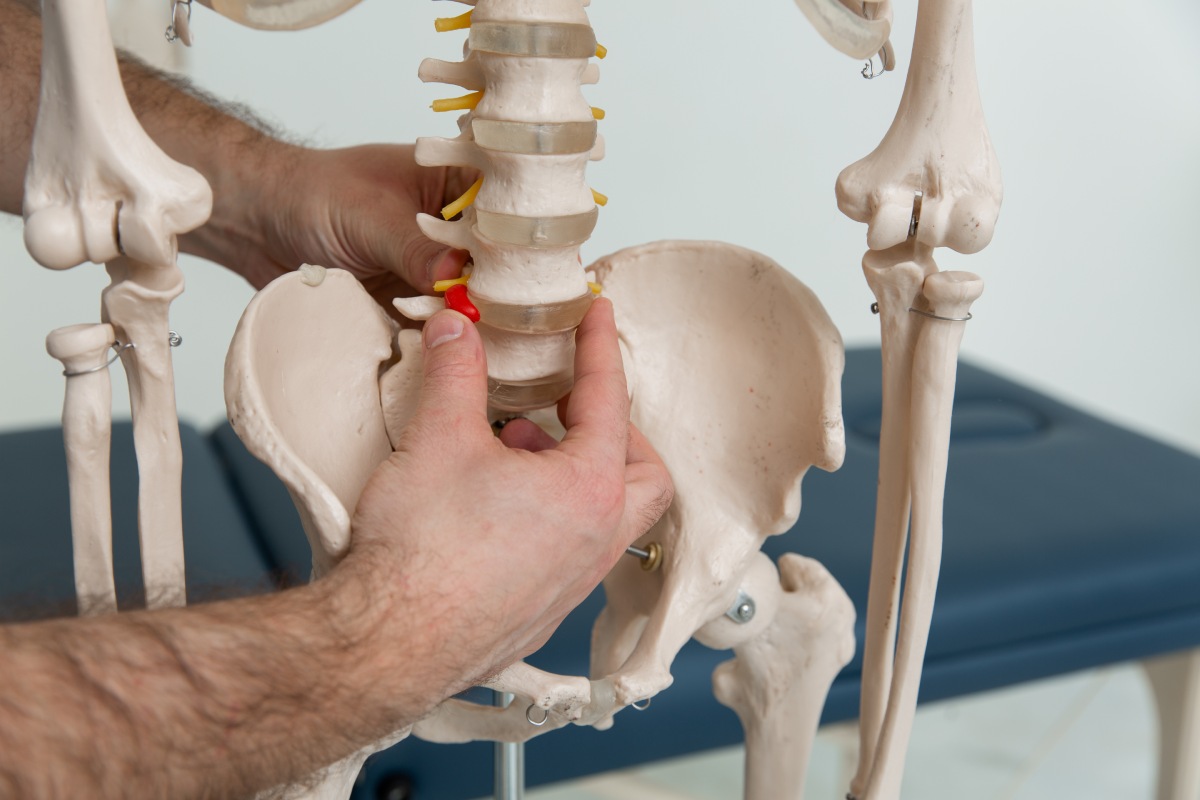
Cervical spine fusion and cervical disc replacement are popular treatments for neck pain and radicular pain (nerve pain into our extremities), the latter having had proven results for several decades. The goal of any spine surgery is relieve pressure that is present on our spinal cord and nerves. With relief of pressure on our nervous system, pain reduction can be achieved.
Keep reading to learn more about both spinal procedures, and recovery.
What is Cervical Disc Replacement Surgery?
Cervical disc replacement removes your cervical disc and replaces it with an artificial one. Replacement surgery is an alternative to cervical spine fusion. As most spine surgeons prefer an anterior approach to the cervical spine (going through the front of the neck), in order to achieve decompression of our nerve and spinal cord for pain relief, typically the entire diseased disc space that is targeted for surgery must be removed.
How serious is cervical disc replacement?
I counsel all of my patients that there is no such thing as minor spine surgery. While we are performing lumbar spine surgeries through 1″ incisions or smaller and performing this surgery through about a 1-1/2″ incision, we are still working around important anatomic structures – especially in the cervical spine. We are exposing your carotid artery and esophagus to mobilizing them to gain visualization to your spine. After that process, we are removing your entire disc to gain direct visualization of your spinal cord.
Therefore, while this surgery only takes about 60-90 minutes and is completed through a small incision, it is still a serious treatment decision.
The Cervical Disc Replacement Surgery Process
Surgeons treat patients with symptoms – not imaging study results. If you have significant pain that is affecting your quality of life, activities of daily living, hobbies, sleep, etc., and have failed reasonable conservative care with time, physical therapy, medications, and/or injections, surgery can become reasonable.
How do I prepare for Cervical Disc Replacement Surgery?
Your doctor will provide specific recommendations as you prepare for your procedure. However, as a general rule, if you take NSAIDs (anti-inflammatories) or anticoagulation medication, you will need to stop these medications 1 week prior to surgery.
Before stopping an anticoagulation medication, it is best to consult with the prescribing provider. They may say it is not safe to stop this anticoagulation medication, which will result in delay or potentially cancellation of your surgery.
What happens during Cervical Disc Replacement Surgery?
The first portion of an artificial disc replacement surgery is identical to fusion surgery. Your surgeon will make an anterior approach to the cervical spine and identify the diseased disc space presumed to be the pain generator based on the preoperative history provided by the patient, physical examination, and MRI evaluation.
After the disc space is properly identified in the operating room, the diseased disc is removed entirely. Again, by removing this disc space, your surgeon will have direct visualization of the spinal cord and nerve roots at this operative level. Your surgeon will work to obtain excellent decompression of the nerves at this level. The void or cavity now present at this disc space level is where your surgeon will implant an artificial disc.
What if your surgeon can’t complete your disc replacement?
In the event the artificial disc is unable to be safely placed during the surgery, your surgeon will automatically convert the surgery into a cervical spine surgery while in the operating room. Fortunately, this is a very rare situation.
I once had a patient whose anatomy just could not conform to prosthesis; therefore, I was forced to transition the surgery to a fusion. While this individual was obviously disappointed with the change is surgical plan, it was the safe and appropriate option for patient care, and their pain was still improved after surgery. However, your surgeon should always counsel you preoperatively about this very small possibility.
How do I recover from Cervical Disc Replacement Surgery?
From an activity standpoint, I encourage walking after surgery. I encourage patients to walk 10 minutes 10 times per day at a comfortable pace. Walking is shown to be the best medication for prevention of postoperative pneumonia and prevention of blood clots. Additionally, regular activity with walking is shown to reduce post operative pain.
Some people wonder whether they should use a cervical collar after surgery. There is no evidence that the use of postoperative cervical collar changes the success / outcome of these surgeries. Therefore, I do not utilize them post-operatively.
What is the success rate of cervical disc replacement surgery?
The most common indication for cervical disc replacement surgery or cervical spine fusion is cervical radiculopathy (nerve pain in our arm(s)). Both procedures have studies showing 80-90% of post operative patients report excellent relief of this pain syndrome.
Who is not a good candidate for cervical disc replacement?
According to the FDA, artificial cervical disc replacement is contraindicated in the following cases:
- Rheumatoid arthritis
- Pregnancy
- Morbid obesity
- Significant osteoporosis
- An active malignancy
- Insulin-dependent diabetes
- Allergies to stainless steel
- An active infection in the body or at the location on the body where surgery will take place
- Other contraindications include:
- Children
- Abnormal motion or instability at the affected level
- Advanced degenerative changes known as spondylosis affecting the facet joints in the back of the spine at the affected level
- Developmental cervical spinal stenosis
- Total loss of disc space
- OPLL (Ossification of the Posterior Longitudinal Ligament)
- Ossification of the ligamentum flavum or main compressive factors located at the dorsal of the spinal cord
Frequently, prior to a general anesthesia event necessary for surgery, a “medical” clearance is requested for the anesthesiologist. With this process, typically some basic laboratory values are obtained from our blood, a chest x-rays is performed, and an electrocardiogram (ECG or EKG) is completed. If a patient has a significant medical history, specialty clearance and review may be required as well (most frequently a cardiologist for a cardiac history).
What should I expect after cervical disc replacement surgery?
The most common complaints after surgery are difficulty swallowing, weak or raspy voice, and surgical site pain. Difficulty swallowing and weak or raspy voice are attributed to the surgical approach. Your surgeon will have to mobilize and retract against your esophagus and throat to visualize the cervical spine. In nearly everybody, both of these complaints completely resolve. However, everyone should expect to experience these symptoms after this surgery. These complaints may resolve in as little as a couple days or continue for several weeks, but we do expect it to improve and resolve in nearly all patients.
Surgical site discomfort is expected after surgery. While the surgical approach is through the front of the neck, patient’s experience pain after surgery most commonly in the back of the neck.
More Cervical Disc Replacement FAQs
What is the difference between Cervical Disc Replacement and cervical fusion?
Once the patient has elected for surgery with the help of a medical professional, they have to decide if fusion surgery or artificial disc replacement surgery is right for them. As stated above, there are positives and negatives to each approach.
The success rates for fusion surgery are very consistent, and it is still considered the “gold standard” for treatment. However, it has a drawback referred to as “adjacent segment degeneration”. Following a fusion surgery, the operative level never moves again – forever. Therefore, the adjacent segment disc spaces attempt to compensate for the loss of motion from the fused spine segment.
As a result of this “extra work”, by these adjacent disc spaces, there is an increased rate of wear or degeneration identified. 10 years after a fusion surgery, 20-25% patients have developed symptomatic adjacent segment degeneration. Therefore, despite the excellent success rates related to pain relief initially after cervical spine fusion surgery, there is certainly caution reserved with regards to long term outcomes and the potential need for further surgery in the future.
The first portion of an artificial disc replacement surgery is identical to fusion surgery. Your surgeon will make an anterior approach to the cervical spine and identify the diseased disc space presumed to be the pain generator based on the preoperative history provided by the patient, physical examination, and MRI evaluation. After the disc space is properly identified in the operating room, the diseased disc is removed entirely.
Instead of proceeding with a fusion reconstruction, your surgeon will implant an artificial disc. The artificial disc consists of 2 separate titanium end plates that bond to the cervical vertebrae with a mobile bearing surface between the end plates to allow for maintenance of the natural motion of the cervical spine disc segment. Because this motion is maintained, the rate of “adjacent segment degeneration” is remarkably improved with studies indicating only about 2-3% of patients have developed adjacent segment degeneration 10 years after surgery. The relief of a patient’s pain and symptoms after artificial disc replacement is found to be similar or near equivalent to pain relief provided after cervical fusion surgery.
The next logical question is, “why wouldn’t everyone want artificial disc replacement surgery instead of fusion?” Well, the technology is still “young” by comparison to fusion. Fusion surgery has been around for many decades with very reproducible results. Artificial disc replacement has been performed in Europe for nearly 30 years, but it has only been approved by the US FDA for about 15 years. While there is very consistent positive data published for artificial disc replacement at 10 years and beyond, it is really difficult to counsel patients about the long term results of the surgery.
How long does a cervical disc replacement last?
Total hip replacement and total knee replacement have been around for many decades, and we know that, eventually, these total hips and knees (with their moving components) wear out and need to be replaced. As the basis of disc replacement technology is similar to total hips and total knees, we do not know exactly when (or if) the artificial disc components will wear out and/or fail. While we are able to replace these moving components in total hips and total knees, this is not possible in the cervical spine. Therefore, when that day comes for a patient, it most certainly will result in a fusion surgery at that time.
What can you not do after cervical spine surgery?
As a general rule after surgery, I recommend no work after surgery for 4-6 weeks with a return to light duty at that time. This is followed by a return to full work duty by 2-3 months. However, I have people with sedentary occupations back to work in less than 1 week. You should not drive a car until you require no sedating medication to control pain. Additionally, you should feel you have a safe and painless range of motion of your cervical spine to fulfill safe driving duties – most people feel comfortable enough with this after a couple of weeks.
Meet Dr. Charles Nalley
Dr. Nalley‘s interests include all aspects of the spine – cervical, thoracic, and lumbar spine disorders including the pelvis / sacroiliac joint. His treatment interests and specialties include operative and non-operative treatment of the spine, and surgical interests include robotic and computer navigated spine surgery.
Make an appointment to see a spinal specialist at Alexander Orthopaedics to answer all of your questions about spinal pain and treatment options
